Are Ozempic and Weight Loss Injections Really the Answer?
- JDR nutrition

- Jan 4
- 4 min read
Updated: Jan 6
Weight loss injections have become one of the most talked-about developments in modern weight management. For many, they appear to offer something dieting has failed to deliver: reduced appetite without constant hunger.
What is often missing from the conversation is a clear explanation of how these medications work, why responses vary so widely, and why appetite suppression alone does not guarantee sustainable weight loss or improved metabolic health. Without this context, expectations are frequently misplaced.

What Weight Loss Injections Actually Do
Medications such as Ozempic, Wegovy and Mounjaro belong to a class of drugs known as GLP-1 receptor agonists, with tirzepatide also acting on GIP receptors.
They mimic endogenous gut hormones involved in appetite regulation and glucose homeostasis. Their primary physiological effects include reduced appetite, earlier satiety and delayed gastric emptying. Weight loss occurs largely because total energy intake decreases, rather than because underlying metabolic dysfunction has been resolved (Wilding et al., 2021; Jastreboff et al., 2022).
Why Weight Loss Outcomes Vary Considerably
Clinical trials typically report average weight loss outcomes, but averages conceal substantial inter-individual variation. In real-world settings, some individuals experience significant weight loss, others achieve modest results, and a proportion lose little or no weight.
Differences in insulin resistance, baseline muscle mass, sleep quality, stress exposure, diet quality and hormonal status all influence response (Hall & Kahan, 2018; Bray et al., 2016). In midlife women, particularly during perimenopause and menopause, aggressive appetite suppression may increase physiological stress and contribute to fatigue, loss of lean mass and metabolic adaptation (Lovejoy et al., 2008; Mauvais-Jarvis et al., 2017).
Weight regulation is not solely a matter of eating less; it is governed by complex biological systems.
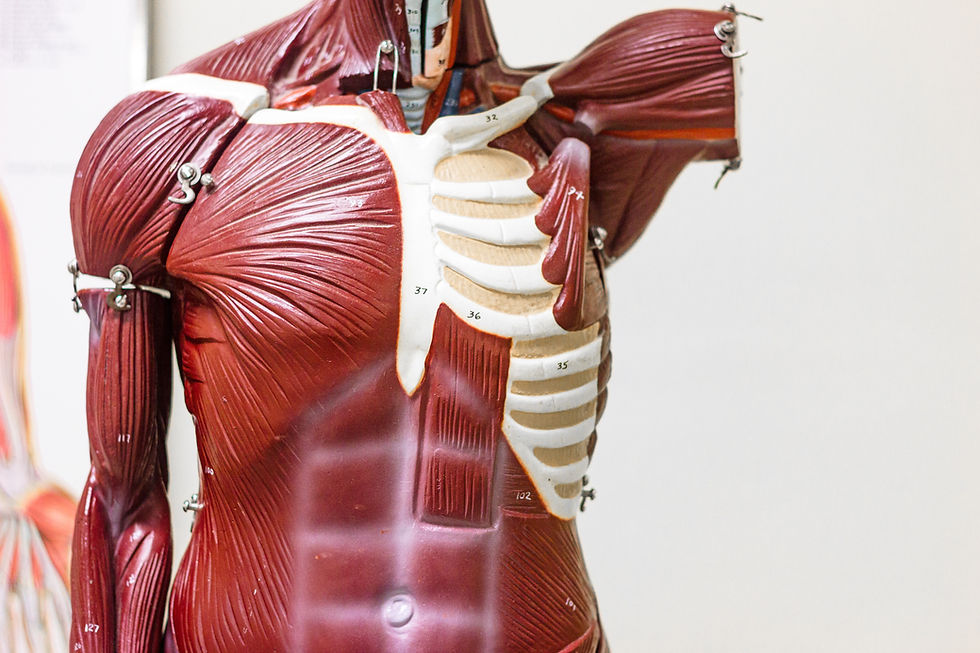
Weight Loss & Muscle Loss: A Key Clinical Concern
Rapid weight loss driven by appetite suppression frequently includes loss of lean body mass. This has important metabolic consequences.
Skeletal muscle is a major determinant of resting metabolic rate and glucose disposal. When calorie intake falls sharply, particularly in the absence of adequate protein intake and resistance training, lean mass loss accelerates (Weinheimer et al., 2010; Heymsfield et al., 2014). This helps explain early weight-loss plateaus, reduced energy expenditure and the high likelihood of weight regain once treatment stops.

Weight Loss & Diet Quality and Nutrient Intake
A suppressed appetite does not guarantee adequate nutrition. When overall intake is low, dietary variety often narrows, increasing the risk of insufficient micronutrient intake.
Over time, this may contribute to fatigue, impaired concentration, hair thinning, reduced immune resilience and poor sleep quality. These effects are more likely when intake is dominated by ultra-processed foods, even in smaller quantities (Hall et al., 2019; Calder et al., 2020).

Duration of Use and Weight Regain
Within UK weight management services, GLP-1-based therapies are reviewed regularly and are not intended as indefinite stand-alone interventions. Evidence consistently shows that weight regain is common following cessation unless changes in diet quality, physical activity and muscle preservation have been implemented alongside pharmacotherapy (Rubino et al., 2021; Sjöström et al., 2017).
This pattern reflects predictable biological adaptation rather than lack of adherence or motivation.
Weight Loss Injections - Side Effects and Safety Considerations
The most commonly reported adverse effects include nausea, vomiting, diarrhoea and constipation. More serious risks such as gallbladder disease and pancreatitis are recognised (Davies et al., 2021).
There has also been recent regulatory attention on rare visual complications, including non-arteritic anterior ischaemic optic neuropathy. While causality has not been definitively established, pharmacovigilance monitoring continues, reinforcing the need for appropriate medical oversight (MHRA Drug Safety Update, 2023).

Cost and Practical Implications of Weight Loss Injections
When self-funded, weight loss injections can cost several thousand pounds per year. This typically excludes nutritional therapy, metabolic assessment, resistance training guidance or structured plans for discontinuation.
For many individuals, the financial commitment persists beyond the point of meaningful benefit.
Weight Loss & Individualised Metabolic Health as the Missing Piece
There is no single intervention that works for everybody. Long-term weight management is shaped by blood glucose regulation, insulin sensitivity, muscle mass, hormonal status, sleep quality and stress physiology.
This is why one-size-fits-all approaches, whether slimming clubs, generic diets or medication alone, often fail to deliver durable results.
Personalised nutritional therapy focuses on improving metabolic health first. Weight loss follows as a downstream effect rather than a constant struggle.
Final Thought
Weight loss injections may reduce hunger, but they do not teach the body how to regulate energy, preserve muscle or maintain health long term.
Sustainable weight loss requires an approach tailored to the individual, grounded in metabolic health rather than appetite suppression alone.
If you are considering weight loss injections, or already using them, working alongside a practitioner to address nutrition, muscle preservation and metabolic resilience can make the difference between short-term weight loss and lasting change.
I Can Help - If you’d like to discuss and individualised plan to support your winter metabolic health naturally, book a free, complimentary chat with me, click below, select a time and I will phone you at the time you choose.
If you enjoyed this article and found it useful, please follow me on Instagram for more health tips
Judith Davis Roach ~ Nutritional Therapist, NLP Coach (@jdr_nutrition) • Instagram photos and videos
References
Bray, G. A., et al. (2016). The science of obesity management: An endocrine perspective. Endocrine Reviews.
Calder, P. C., et al. (2020). Nutrition and immune function. BMJ.
Davies, M., et al. (2021). Semaglutide in adults with overweight or obesity. New England Journal of Medicine.
Hall, K. D., et al. (2019). Ultra-processed diets cause excess calorie intake and weight gain. Cell Metabolism.
Hall, K. D., & Kahan, S. (2018). Maintenance of lost weight and long-term management of obesity. Medical Clinics of North America.
Heymsfield, S. B., et al. (2014). Energy content of weight loss: kinetic features. American Journal of Clinical Nutrition.
Jastreboff, A. M., et al. (2022). Tirzepatide once weekly for the treatment of obesity. New England Journal of Medicine.
Lovejoy, J. C., et al. (2008). Weight gain in women at midlife. Obesity.
Mauvais-Jarvis, F., et al. (2017). Sex and gender: modifiers of health, disease, and medicine. Lancet.
Rubino, D., et al. (2021). Weight regain after withdrawal of semaglutide. Diabetes, Obesity and Metabolism.
Sjöström, L., et al. (2017). Effects of bariatric surgery on mortality. New England Journal of Medicine.
Weinheimer, E. M., et al. (2010). Lean mass loss during weight loss. Obesity Reviews.
Wilding, J. P. H., et al. (2021). Once-weekly semaglutide in adults with overweight or obesity. New England Journal of Medicine.
MHRA Drug Safety Update. (2023). GLP-1 receptor agonists: ongoing safety monitoring.




Comments